Achilles Tendonitis Doesn’t Have To Keep You Sidelined
July 11, 2019 · Julian Corwin
“There are plenty of difficult obstacles in your path. Don’t allow yourself to become one of them.” – Ralph Marston
One of the most debilitating obstacles that can slow down or sidetrack us is an injury. Sometimes it is sudden and can be associated with a specific event or action. At other times, it can simply be the result of long involvement in active sports, the rigors of our work and everything else in life that causes our bodies to gradually weaken.
For most people, pain and injuries can cause them to slow down or even seek medical help. For others, however, they choose to ignore the pain and discomfort. This is especially true for more athletic types who tend to push through the pain. The problem with that approach is that, if the pain is the result of an injury or actual damage of the body, this will simply cause more damage.
And a common affliction for many athletes is Achilles Tendonitis. This is especially true for those between 30 to 40 who are involved in sports that involve running, jumping, and sudden starts and stops such as soccer, basketball and tennis. And an Achilles tendon rupture is almost five times more likely to occur in men than in women.
Achilles Tendonitis Symptoms and Diagnosis
According to the Mayo Clinic’s website Achilles Tendinitis is described as,
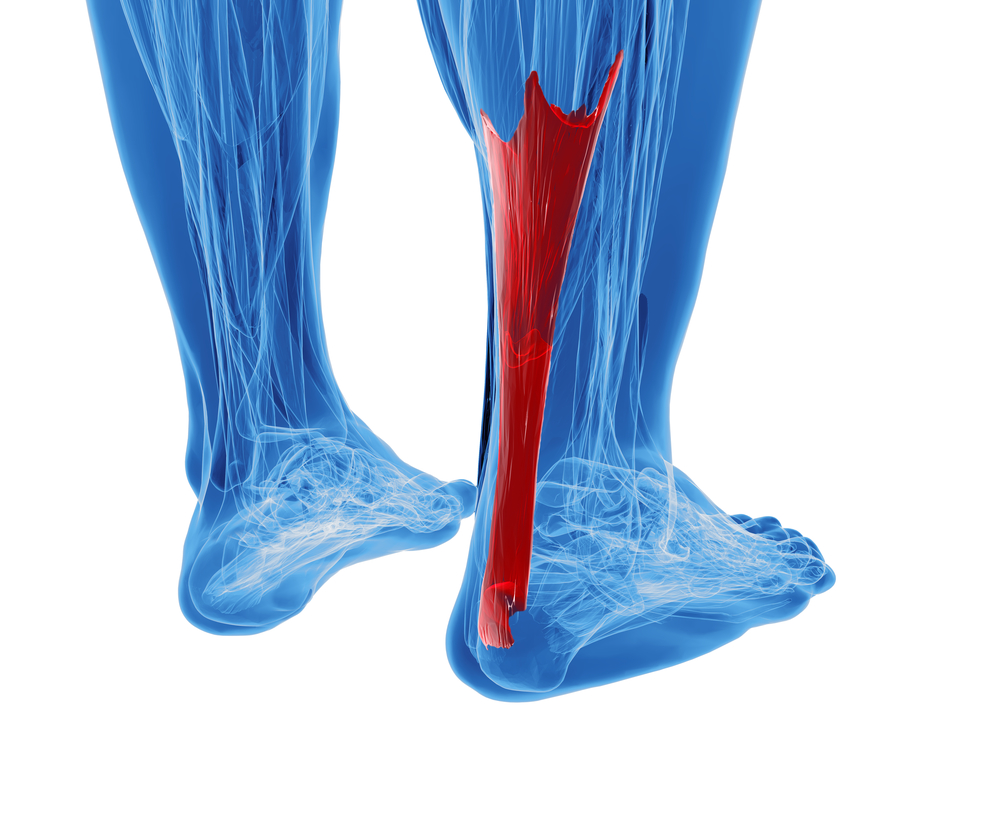
“[A]n overuse injury of the Achilles (uh-KILL-eez) tendon, the band of tissue that connects calf muscles at the back of the lower leg to your heel bone. Achilles tendinitis most commonly occurs in runners who have suddenly increased the intensity or duration of their runs. It’s also common in middle-aged people who play sports, such as tennis or basketball, only on the weekends.”
The blood supply for the Achilles tendon comes from the muscles above it and from the bony attachment below, known as the calcaneus, or heel bone. Paratenonitis, when the tendon rubs over the bone, and tendinosis usually develop in the area approximately one to four inches above the heel bone.
Treating your Achilles Tendonitis can start once we learn your symptoms and we can diagnose it.
The symptoms typically begin gradually and seemingly spontaneously. Aching and burning pain are noted especially with morning activity. It may improve slightly with initial activity but becomes worse with further activity. It is aggravated by exercise. Over time less exercise is required to cause the pain. There may be a weakness in push-off strength with walking.
Often, too, the Achilles tendon will be enlarged and feel warm and tender to the touch. Sometimes friction is noted with gentle palpation of the tendon during ankle motion. Paratenonitis is more common in those under 30, while tendonitis has similar symptoms but is more typical in middle-aged people. If the pain is severe pain and walking is difficult, this could indicate a partial tear of the Achilles tendon.
The Common Treatments for Achilles Tendonitis
There are two approaches to treating Achilles tendonitis. These can be referred to as Non-surgical and Surgical treatments. While most cases can be successfully treated non-surgically , it is a lengthy process and can be quite frustrating for very active patients. Non-surgical treatments are less likely to be successful, however, if the condition has been present six months or more.
Non-surgical treatment regimens can include nonsteroidal anti-inflammatory medications such as aspirin or ibuprofen, immobilization, limitation of activity, regulated rest, ice application, contrast baths, stretching and heel lifts. An arch support can also be used if pes planus or fallen arches, also known as flat feet, is an issue.
In some instances, a cast or brace may be required to completely rest this area. In addition, some success has been associated with extracorporeal shockwave therapy, platelet-rich plasma injections and nitroglycerin medication applied to the overlying skin.
When non-invasive treatments like those described fail to repair the scar tissue, surgical treatment for Achilles tendonitis is an option.
Typically, the surgical approach consists of excising any scar tissue and calcification deposits within the Achilles tendon. Any abnormal tissue present is gradually removed until tissue with normal appearance is exposed. The tendon is then repaired with sutures.
Fortunately for some, the Achilles tendon repair surgery can be done as a minimally invasive procedure. This is accomplished with several small incisions instead of one large incision. If needed, a special scope with a tiny camera and a light can be used, as well, to help complete the tendon repair.
If a patient is elderly, or in those cases when more than 50 percent of the tendon must be removed, the surgeon might replace part or all the Achilles tendon. This is done with a tendon taken from another place in the foot or calf.
Hopkins Medicine nots the potential risks of Achilles tendon repair surgery,
“Every surgery has risks. Risks of Achilles tendon repair include:
- Excess bleeding
- Nerve damage
- Infection
- Blood clot
- Wound healing problems
- Calf weakness
- Complications from anesthesia
- Continued pain in your foot and ankle
Your own risks may vary according to your age, the shape of your foot and leg muscles and tendons, your general health, and the type of surgery done. Talk to your healthcare provider about any concerns you have. He or she can tell you the risks that most apply to you.”
Keep Moving With Pain and Performance Solutions
When treating any injury or issues causing chronic pain, it’s important to have patience. Because time is what’s needed for complete healing. We stress this because we’ve seen too many people rush back into their work or sports activity before they are completely healed.
Treating your Achilles Tendonitis is just like treating any other injury: it simply can’t be rushed. The reality is that you’ll probably do more damage and possibly never recover fully.
Here at Pain and Performance Solutions we can help you by treating your Achilles Tendonitis, so please reach out to us today. You can contact us at (707) 636-4404 and Let’s start the healthy journey back to your body’s ultimate healthy state.